Abstract
Introduction and hypothesis
This study is about evaluating safety and potential risk factors for complications following pelvic organ prolapse repair with the GYNECARE PROLIFT system.
Methods
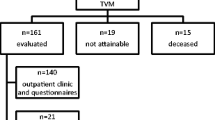
This is a prospective observational study (Canadian Task Force II-1) performed in a tertiary referral center. A total of 114 women with pelvic organ prolapse, POP-Q stage ≥2, underwent a pelvic floor repair that included Prolift.
Results
During a mean follow-up time of 7 months there were six procedure failures (5.3%) and 14 mesh exposures (12.3%), more commonly on the anterior vaginal wall. Age was inversely related to the risk of having late mesh exposure (p = 0.02) with an odds ratio of 1.99 (95% confidence interval 1.10–3.59) for each decrease of 10 years in age. Late mesh exposure was significantly more common in sexually active patients (p = 0.016).
Conclusions
Prolift repair has a high anatomical success rate. Young age and sexual activity are risk factors for mesh exposure.
Similar content being viewed by others
Abbreviations
- POP:
-
Pelvic organ prolapse
- TVM:
-
Transvaginal mesh repair
References
Olsen AL, Smith VJ, Bergstrom JO et al (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89:501–506
Chen CC, Ridgeway B, Paraiso MF (2007) Biologic grafts and synthetic meshes in pelvic reconstructive surgery. Clin Obstet Gynecol 50(2):383–411
Maher C, Baessler K, Glazener CMA, Adams EJ, Hagen S (2007) Surgical management of pelvic organ prolapse in women. Cochrane Database of Systematic Reviews (3):CD004014
Amid P (1997) Classification of biomaterials and their related complications in abdominal wall surgery. Hernia 1:15–21
Debodinance P, Berrocal J, Clave H et al (2004) Changing attitudes on the surgical treatment of urogenital prolapse: birth of the tension-free vaginal mesh. J Gynécol Obstét Biol Reprod 33(7):577–588
Collinet P, Belot F, Debodinance P et al (2006) Transvaginal mesh technique for pelvic organ prolapse repair: mesh exposure management and risk factors. Int Urogynecol J 17:315–320
National Institute for Health and Clinical Excellence (2008) Surgical repair of vaginal wall prolapse using mesh. Interventional procedure guidance 267. London, UK
Fatton B, Amblard J, Debodinance P, Cosson M, Jacquetin B (2007) Transvaginal repair of genital prolapse: preliminary results of a new tension-free vaginal mesh (Prolift™ technique)—a case series multicentric study. Int Urogynecol J 18:743–752
Gauruder-Burmester A, Koutouzidou P, Rohne J, Gronewold M, Tunn R (2007) Follow-up after polypropylene mesh repair of anterior and posterior compartments in patients with recurrent prolapse. Int Urogynecol J 18:1059–1064
Baessler K, O’Neill SM, Maher CF, Battistutta D (2009) Australian pelvic floor questionnaire: a validated interviewer administered pelvic floor questionnaire for routine clinic and research. Int Urogynecol J Pelvic Floor Dysfunct 20:149–158
Digesu GA, Khullar V, Cardozo L, Robinson D, Salvatore S (2005) P-QOL: a validated questionnaire to assess the symptoms and quality of life of women with urogenital prolapse. Int Urogynecol J 16:176–181
Rogers RG, Coates KW, Kammerer-Doak D, Khalsa S, Qualls C (2003) A short form of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire (PISQ-12). Int Urogynecol J 14(3):164–168
Bump RC, Mattiasson A, Bo K et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–11
Carey M, Higgs P, Goh J, Lim J, Leong A, Krause H, Cornish A (2009) Vaginal repair with mesh versus colporrhaphy for prolapse: a randomised controlled trial. BJOG 116(10):1380–1386
Nguyen JN, Burchette RJ (2008) Outcome after anterior vaginal prolapse repair: a randomized controlled trial. Obstet Gynecol 111(4):891–898
Mistrangelo E, Mancuso S, Nadalini C, Lijoi D, Constantini S (2007) Rising use of synthetic mesh in transvaginal pelvic reconstructive surgery: a review of the risk of vaginal erosion. JMIG 14:564–569
Deffieux X, de Tayrac R, Huel C, Bottero J, Gervaise A et al (2007) Vaginal mesh erosion after transvaginal repair of cystocele using Gynemesh or Gynemesh-Soft in 138 women: a comparative study. Int Urogynecol J 18:73–79
Achtari C, Hiscock R, O’Reilly BA, Schierlitz L, Dwyer PL (2005) Risk factors for mesh erosion after transvaginal surgery using polypropylene (Atrium) or composite polypropylene/polyglactin 910 (Vypro II) mesh. Int Urogynecol J 16:389–394
Milani R, Salvatore S, Soligo M, Pifarotti P, Meschia M, Cortese M (2005) Functional and anatomical outcome of anterior and posterior vaginal prolapse repair with prolene mesh. BJOG 112:107–111
Dwyer PL, O’Reilly BA (2004) Transvaginal repair of anterior and posterior compartment prolapse with Atrium polypropylene mesh. BJOG 111:831–836
Danielsson I, Sjöberg I, Stenlund H, Wikman M (2003) Prevalence and incidence of prolonged and severe dyspareunia in women: results from a population study. Scand J Public Health 31:113–118
Acknowledgments
We wish to acknowledge the help of Dr. Georgina Luscombe who assisted with the statistical analysis.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaufman, Y., Singh, S.S., Alturki, H. et al. Age and sexual activity are risk factors for mesh exposure following transvaginal mesh repair. Int Urogynecol J 22, 307–313 (2011). https://doi.org/10.1007/s00192-010-1270-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-010-1270-6