Relation of infant diet to childhood health: seven year follow up of cohort of children in Dundee infant feeding study
BMJ 1998; 316 doi: https://doi.org/10.1136/bmj.316.7124.21 (Published 03 January 1998) Cite this as: BMJ 1998;316:21- Andrea C Wilson, research dietitian, child healtha,
- J Stewart Forsyth, consultant paediatriciana (stewart.f{at}dth.scot.nhs.uk),
- Stephen A Greene, consultant paediatriciana,
- Linda Irvine, research nurse, child healtha,
- Catherine Hau, statisticiana,
- Peter W Howie, professor of obstetrics and gynaecologya
- a Departments of Child Health, Epidemiology and Public Health, and Obstetrics and Gynaecology, Ninewells Hospital and Medical School, Dundee DD1 9SY
- Correspondence to: Dr Forsyth
- Accepted 26 August 1997
Abstract
Objective: To investigate the relation of infant feeding practice to childhood respiratory illness, growth, body composition, and blood pressure.
Design: Follow up study of a cohort of children (mean age 7.3 years) who had detailed infant feeding and demographic data collected prospectively during the first two years of life.
Setting: Dundee.
Subjects: 674 infants, of whom 545 (81%) were available for study. Data on respiratory illness were available for 545 children (mean age 7.3 (range 6.1- 9.9) years); height for 410 children; weight and body mass index for 412 children; body composition for 405 children; blood pressure for 301 children (mean age 7.2 (range 6.9-10.0) years).
Main outcome measures: Respiratory illness, weight, height, body mass index, percentage body fat, and blood pressure in relation to duration of breast feeding and timing of introduction of solids.
Results: After adjustment for the significant confounding variables the estimated probability of ever having respiratory illness in children who received breast milk exclusively for at least 15 weeks was consistently lower (17.0% (95% confidence interval 15.9% to 18.1%) for exclusive breast feeding, 31.0% (26.8% to 35.2%) for partial breast feeding, and 32.2% (30.7% to 33.7%) for bottle feeding. Solid feeding before 15 weeks was associated with an increased probability of wheeze during childhood (21.0% (19.9% to 22.1%) v 9.7% (8.6% to 10.8%)). It was also associated with increased percentage body fat and weight in childhood (mean body fat 18.5% (18.2% to 18.8%) v 16.5% (16.0% to 17.0%); weight standard deviation score 0.02 (−0.02 to 0.06) v −0.09 (−0.16 to 0.02). Systolic blood pressure was raised significantly in children who were exclusively bottle fed compared with children who received breast milk (mean 94.2 (93.5 to 94.9) mm Hg v 90.7 (89.9 to 91.7) mm Hg).
Conclusions: The probability of respiratory illness occurring at any time during childhood is significantly reduced if the child is fed exclusively breast milk for 15 weeks and no solid foods are introduced during this time. Breast feeding and the late introduction of solids may have a beneficial effect on childhood health and subsequent adult disease.
Key messages
Current guidelines in the United Kingdom recommend that babies are exclusively breast fed for the first 4 months of life, with solids being introduced thereafter
This study found that exclusive breast feeding is associated with a significant reduction in childhood respiratory illness
The early introduction of solids is associated with increased body fat and weight in childhood
Exclusive bottle feeding is associated with higher systolic blood pressure in childhood
Breast feeding and delaying the introduction of solids until after 15 weeks may have a beneficial effect on childhood health and subsequent adult disease
Introdution
The extent to which adult health is determined by nutritional factors in early life has been the subject of much debate since Barker observed that low birth weight and weight at 1 year are associated with adult disease.1 One of the explanations for these findings is that nutritional deficiencies at critical periods of fetal and infant growth may induce permanent changes in physiological function.2 Whether infant feeding practice influences childhood or adult health remains uncertain. Breast feeding is associated with health gain during infancy, with reduction in gastroenteritis and respiratory disease,3 but whether these benefits extend into childhood has not been established. Infant feeding practice varies widely throughout the United Kingdom. Exclusive breast feeding is recommended for at least four months, with solid foods being introduced thereafter,4 5 but currently in the United Kingdom 64% of infants are breast fed initially, with only 19% still being breast fed at 4 months of age. Additionally, 90% of infants start eating solid foods before the age of 4 months.6 With this variance between recommendation and practice, robust evidence is needed to support the national policy. We determined the relation between infant feeding practice and childhood health. Outcome measures were episodes of respiratory illness and measurements of growth, body composition, and blood pressure. Infant feeding data from the first two years of life were collected prospectively as part of the Dundee infant feeding study.3
Subjects and methods
The parents or guardians of the 674 children recruited to the original Dundee infant feeding study during September 1983 to May 19863 were contacted by letter from September 1990 to December 1993. Demographic, clinical, and feeding data had been collected prospectively from birth and at intervals during the first two years. Ethical approval for the study was obtained from Tayside Committee on Medical Ethics. A questionnaire, which was checked during a home visit, was completed by parents on their child's symptoms, diagnoses, and treatment of respiratory illness during the previous 12 months and at any time since birth. Information on family history of atopy and current demographic data were obtained. The questionnaire had minor modifications from that used in a study of asthma in British schoolchildren.7 Respiratory illness included one or more respiratory symptoms (persistent cough, wheeze, or breathlessness as defined in the questionnaire7) at any time since birth (ever) or during the previous 12 months (current). A child was considered to have asthma if a doctor had diagnosed asthma at any time since birth (ever) or if the child was currently receiving asthma treatment (current).
Arrangements were made for several measurements to be taken either at home or in hospital. Children's height, weight, skinfold thickness (at four sites), and bioelectrical impedance and parents' height were measured. Percentage body fat was calculated from skinfold thickness8 and by bioelectrical impedance. Bioelectrical impedance was measured by a Holtain body composition analyser, from which total body water was calculated9 and the percentage of body fat deduced. Blood pressure was measured by a random zero sphygmomanometer: the widest cuff that could be applied to the arm was used, as recommended by the British Hypertension Society.10 Systolic blood pressure was taken as Korotkoff's first phase and diastolic blood pressure as phase V. Not all children in this large follow up cohort study were available for measurement. Blood pressure was not recorded in the initial phase of the study (90 children).
Data on infant feeding were collected prospectively during the first two years of life3 and included duration of breast and formula feeding and the time of introduction of formula feeds and solid foods. From these data three milk feeding groups and two solid feeding groups were identified to reflect current infant feeding practices in the United Kingdom,6 thereby allowing comparison with current national recommendations on infant feeding.4 5 These groups were exclusive breast feeding for at least 15 weeks; partial breast feeding (infant milk supplements before 15 weeks; mean duration of breast feeding 9.5 weeks (95% confidence interval 7.9 to 11.1 weeks)); exclusive bottle feeding; solids introduced before 15 weeks; and solids introduced at 15 weeks or later.
The statistical package for the social sciences (SPSS/PC+) was used for data management and tabulation, and general linear interactive modelling for analysis. The respiratory data were in the form of binary (yes/no) variables and therefore logistic regression was used. Several variables were assessed as potential covariates in the analyses: parental history of asthma was coded into binary variables; social class was coded according to the occupation of the main wage earner into eight categories (I, II, IIIa, IIIb, IV, V, armed forces, and unemployed according to the classification of the Office of Population Censuses and Surveys11; the number of people smoking per household was coded as 0, 1, 2, and 3 or more. Other covariates investigated were birth weight, weight at first solid feed, maternal height, and maternal blood pressure, sex, parity, and gestation. We studied the relation of infant feeding group to prevalence of respiratory illness, growth, body composition, and blood pressure after allowing for significant variables.
Results
From the original cohort of 674 children, 545 (81%) completed questionnaires were received, with 412 of these 545 (75%) having complete physiological, demographic, and feeding data (fig 1). Children were excluded from analysis if they did not have a measurement of maternal height, maternal blood pressure, or weight at first solid feed. Paternal blood pressure was not used in the analysis as it was obtained in only 214 of the families. Analysis of data on children who were not traced or who were excluded from the analysis found no significant differences in birth weight, gestation, parity, or solid feeding group, but there were differences in social class and milk feeding group (see below).
Numbers of children with complete feeding data and in whom anthropometric data were analysed
Respiratory data
Table 1 shows the characteristics of the population within each of the milk feeding groups. Nineteen per cent (129) of the original cohort were not available for respiratory analysis: 55 were bottle fed (21% of the original bottle feeding group), 39 (16%) were partially breast fed, and 23 (14%) were exclusively breast fed. Twelve children had insufficient data to be placed in a feeding group. Proportionally more of the children who were not followed up were in social class IV but proportionally fewer children had parents who were unemployed.
Characteristics of 545 children followed up at mean age of 7.3 years according to type of milk feeding in infancy. Values are numbers (percentages) of children
Three variables had a significant relation to the outcome of respiratory illness: socioeconomic group, family history of atopy, and sex of the child. These variables were adjusted for in the logistic regression analysis of the relation of respiratory illness and associated symptoms to infant feeding. The estimated probabilities of respiratory symptoms ever occurring differed significantly between the milk feeding groups. The estimated probability of ever having respiratory illness was consistently lower in the children who had received breast milk exclusively for 15 weeks or more (estimated probability was 17.0% (95% confidence interval 15.9% to 18.1%) for exclusive breast feeding, 31.0% (26.8% to 35.2%) for partial breast feeding, and 32.2% (30.7% to 33.7%) for bottle feeding). The estimated probability of ever having cough was also consistently lower in this group (11.3% (10.7% to 11.9% for exclusive breast feeding, 22.2% (19.5% to 24.9%) for partial breast feeding, and 24.6% (23.6% to 25.6%) for bottle feeding) (table 2). Similar associations were seen for current respiratory symptoms, with a lower estimated probability of respiratory illness and cough (data not shown).
Estimated percentage probabilities (95% confidence intervals) of the 545 children ever having respiratory symptoms according to feeding group and after adjustment for parental history of atopic disease, sex, and social class
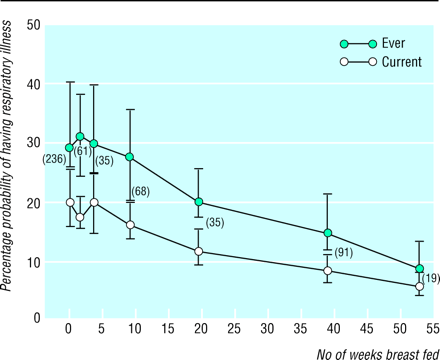
Early solid feeding (solids before 15 weeks) was associated with an increased probability of wheeze during childhood: 21.0% (19.9% to 22.1%) in those who had solids before 15 weeks v 9.7% (8.6% to 10.8%) in those who had solids after 15 weeks. We found no significant relation with maternal or paternal smoking after adjustment for the effect of solids. The probability of ever having or currently having asthma was not significantly different between the feeding groups. Data on respiratory illness were also analysed using infant feeding as a continuous variable. The results were similar, with a longer duration of breast feeding being associated with a reduced probability of ever having (P<0.01) or currently (P<0.05) having respiratory illness (fig 2).
Estimated percentage probability of ever having or currently having respiratory illness according to number of weeks of breast feeding. Values are medians and interquartile ranges, with number of children in each time category given in parentheses
Growth and body composition
Table 3 shows physical data for the children (mean age 7.2; range 6.9 to 10.0 years) who had measurements for growth, body composition, and blood pressure. Height, weight, and body mass index are expressed as standard deviation scores calculated from local standards.12 Proportionally more of the children who were not followed up were children in social class IV but proportionally fewer children had parents who were unemployed.
Unadjusted physical data for boys and girls (mean age 7.2 years)
Growth and body composition in childhood were related significantly to several covariables (table 4). After adjustment for these variables (height; maternal height, socioeconomic group, birth weight, and sex; weight, body mass index, and percentage body fat; sex, birth weight, and weight at first solids) the effect of infant feeding was assessed using multiple regression analysis (see table 6). Children who had been given solids before 15 weeks were significantly heavier than those given solids at 15 weeks or later (mean weight standard deviation score 0.02 (−0.02 to 0.06) v −0.09 (−0.16 to 0.02)). The percentage of body fat measured either by skinfold thickness or impedance was significantly greater in the children who had been given solid foods before 15 weeks of age (mean body fat from impedance 18.5% (18.2% to 18.8%) v 16.5% (16.0% to 17.0%)). Body fat was also greater in girls than boys (P<0.01). Body mass index and height were not significantly different between the solid or milk feeding groups. The data were also analysed using infant feeding as continuous variables. This produced similar results, with the percentage of body fat and weight being greater in the children who were introduced to solids earlier.
Univariate analysis of individual predictors of growth and body composition. Values are r2 (P values)
Blood pressure
Systolic and diastolic blood pressure in the children were influenced significantly by body mass index, sex (higher in boys than girls), and maternal blood pressure (table 5). After adjustment for these variables the relation between blood pressure and infant feeding was investigated. Although blood pressure was not available or recorded in 373 (55%) of the original cohort, the distribution of the children among the feeding groups and social class categories was proportionally similar to that for respiratory data.
Univariate analysis of individual predictors of blood pressure. Values are r2 (P values)
Table 6 shows the mean estimated values for blood pressure. Systolic blood pressure in the children was related to the milk feeding groups: children exclusively bottle fed had a higher systolic blood pressure (mean blood pressure 94.2 (93.5 to 94.9) mm Hg in those who were bottle fed, 90.9 (90.2 to 91.6) mm Hg in those who were partially breast fed, and 90.3 (89.5 to 91.1) mm Hg in those who were exclusively breast fed). The mean difference between the bottle fed and the breast fed group was 3 mm Hg, with an increase of 3 mm Hg for each standard deviation score rise in body mass index. Birth weight was not significantly associated with the children's blood pressure after adjustment for current body mass index. Diastolic blood pressure was not influenced by infant feeding after adjustment for confounding variables (maternal blood pressure, body mass index, and sex).
Mean estimated values for weight, body mass index, and percentage body fat (adjusted for sex, birth weight, and weight at first solid feed) and systolic and diastolic pressure (adjusted for sex, body mass index, and maternal blood pressure) in children at mean age 7.2 years according to feeding group
The data were also analysed using breast feeding as a continuous variable. Results were similar, with a longer duration of breast feeding being associated with a reduction in systolic blood pressure in the children.
Discussion
We reported previously that breast feeding for 13 weeks reduced the incidence of gastrointestinal illness and respiratory illness during the first year of life.3 An issue arising from that study was whether the benefits from breast feeding would continue into childhood. This study shows that exclusive breast feeding for at least 15 weeks is associated with a significant reduction in respiratory illness during the first seven years of life, that exclusive formula feeding is associated with a significantly higher blood pressure at the age of 7, and that early solid feeding is associated with increased weight, percentage body fat, and risk of wheezing in childhood. The associations were not only categorical but also continuous, indicating a dose-response effect.
Not all children on whom we had infant feeding data could be recruited to this study, and we noted the differences between the children studied and those who were not recruited from the original cohort. There was a trend towards higher social class and less exclusive bottle feeding in this study group. The effect of these differences on the results is uncertain, but children in our study cohort may have been at lower risk of developing the outcome measures and the results might have been more significant in the complete cohort. With this type of study, the statistical relations reported may be due to factors that were not included in the study, and therefore we must be cautious in drawing conclusions.
Respiratory illness
We did not find an association between parental smoking and respiratory illness. The positive association reported in previous studies may relate to a failure to include the confounding effect of solid feeding on respiratory illness13: when we excluded solid feeding from the regression analysis, respiratory illness was related significantly to parental smoking. We did not find a significant relation between the feeding groups and a diagnosis of asthma, but an early introduction to solids was associated with a history of wheezing. Fergusson et al did not find a relation between the introduction of solids before 4 months of age and asthma at age 4 years.14 The prevalence of asthma in children aged 7 is 20% higher than that in those aged 4,15 and Fergusson et al also included wheezy bronchitis in their asthma group.
The mechanism for the association between breast feeding and the lower probability of respiratory illness is uncertain. In a study comparing soya milk with breast feeding, soya failed to reduce the incidence of wheeze or allergy, whereas the incidence of respiratory symptoms was significantly lower in the breast feeding group.13 The authors concluded that wheeze is more likely to be secondary to infection than due to allergy.13 Our previous study showed a reduction in respiratory illness during the first year of life3 and our current study indicates that the protective effect of breast milk continues into later childhood.
Body composition and blood pressure
We previously reported that formula feeding and timing of solids did not influence weight at the age of 2 years,16 but in our current study the introduction of solids before 15 weeks was associated with heavier and fatter children. We did not observe an effect of birth weight on childhood blood pressure after adjusting for current body mass index. The type of milk feeding did, however, influence blood pressure, with breast feeding being associated with lower systolic pressure. Recent studies of the association of birth weight with childhood and adult blood pressure are conflicting: a study of children aged 6-16 years reported that blood pressure was inversely related to birth weight,17 whereas Whincup et al did not find an effect of birth weight on blood pressure in 10 year old children and suggested that other environmental factors operating in childhood may be more important.18 A high salt intake in adults increases blood pressure.19 In children, however, the data linking diet and blood pressure are limited. One study has shown an association between a high intake of sodium during the newborn period and infant blood pressure,20 while others have not.21 Although some modern infant formulas have a sodium content similar to breast milk, others have a higher content and errors in reconstitution may lead to higher than anticipated intakes of sodium.22 23
In summary, this study indicates that in an industrialised society exclusive breast feeding for at least 15 weeks and the avoidance of solid foods before 15 weeks in healthy term infants may confer significant longterm health benefits on the child. If the hypothesis of programming is correct, the observed differences in body composition and blood pressure may become magnified with time and be important antecedents of adult disease. These data provide clinical evidence to support the current national recommendations for breast feeding and timing of introduction of solids.5
Acknowledgments
Funding: This study was supported by grants from the Scottish Home and Health Department and the Department of Health.
Conflict of interest: None.
Notes
Contributors: ACW, the principal investigator for the study, was involved in the execution of the study, particularly data collection, documentation, and analysis and in writing the paper; she also participated in the design of the study. JSF initiated the Dundee infant feeding study research project and the present project, coordinated the study, and participated in the analysis and interpretation of the data and in writing the paper. SAG initiated the research and participated in the analysis and interpretation of the data and in writing the paper. LI participated in the design of the study and data collection and edited the paper. CH undertook the statistical analysis and edited the paper. PWH initiated the Dundee infant feeding study research project, discussed interpretation of the findings, and edited the paper. SAG and JSF will act as guarantors of the study.