Challenges to implementing the national programme for information technology (NPfIT): a qualitative study
BMJ 2005; 331 doi: https://doi.org/10.1136/bmj.331.7512.331 (Published 04 August 2005) Cite this as: BMJ 2005;331:331- Jane Hendy (jane.hendy{at}lshtm.ac.uk), research fellow1,
- Barnaby C Reeves, reader in epidemiology1,
- Naomi Fulop, senior lecturer in health services delivery and organisational research1,
- Andrew Hutchings, lecturer in health services research1,
- Cristina Masseria, research fellow1
- 1 Department of Public Health and Policy, London School of Hygiene and Tropical Medicine, London WC1E 7HT
- Correspondence to: J Hendy
- Accepted 27 May 2005
Abstract
Objectives To describe the context for implementing the national programme for information technology (NPfIT) in England, actual and perceived barriers, and opportunities to facilitate implementation.
Design Case studies and in depth interviews, with themes identified using a framework developed from grounded theory.
Setting Four acute NHS trusts in England.
Participants Senior trust managers and clinicians, including chief executives, directors of information technology, medical directors, and directors of nursing.
Results The trusts varied in their circumstances, which may affect their ability to implement the NPfIT. The process of implementation has been suboptimal, leading to reports of low morale by the NHS staff responsible for implementation. The overall timetable is unrealistic, and trusts are uncertain about their implementation schedules. Short term benefits alone are unlikely to persuade NHS staff to adopt the national programme enthusiastically, and some may experience a loss of electronic functionality in the short term.
Conclusions: The sociocultural challenges to implementing the NPfIT are as daunting as the technical and logistical ones. Senior NHS staff feel these have been neglected. We recommend that national programme managers prioritise strategies to improve communication with, and to gain the cooperation of, front line staff.
Introduction
In 1998 the NHS Executive set a target for all NHS trusts to have electronic patient records in place by 2005.1 By the spring of 2002, just 3% of trusts were set to meet this target.2 The Treasury's Wanless report suggested two main reasons for this: budgets for information technology (IT), allocated locally, being used to relieve financial pressures elsewhere, and the inadequate setting of central IT standards.3 The report recommended ring fencing and doubling the IT budget. The government responded with £2.3bn ($4.4bn; €3.3bn) for a new national programme for information technology (NPfIT) in the NHS in England.4 The aim is for electronic patient records to be implemented in all acute trusts by the end of 2007.
The size, complexity, and innovation of this national programme (also now called Connecting for Health) makes it the biggest outsourced IT project from the public sector ever untaken.5 Implementing large scale health service IT projects, in the United Kingdom and other countries, has proved difficult.6 7 Problems of achieving effective information flow between users, the cornerstone of any integrated record system, and resolving issues of confidentiality and security have led to reported failure rates of around 30%.8 9 The recent IT implementation failure experienced by the Wessex Regional Health Authority ended in losses to the taxpayer of £43m.5 The NPfIT has been described as “ambitious” and “inherently risky.”10 The National Audit Office is currently evaluating whether the programme is likely to deliver good value for money and reviewing implementation progress.11 A report is due in the summer.
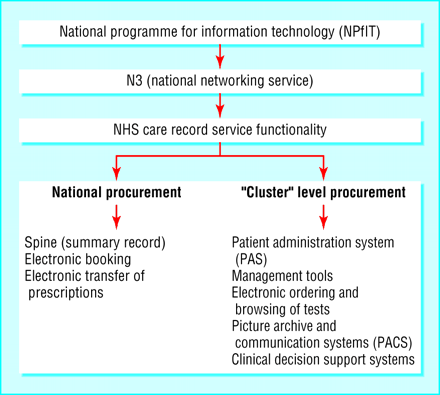
The programme's key features are new stringent national data and IT standards, procured and paid for nationally. Implementation in acute trusts will be through one of five geographic partnerships with industry, called “clusters.” A ministerial taskforce and a NHS IT director general oversee progress. The main national features are a new national networking service providing broadband, called “N3”; electronic booking, called “choose and book”; electronic transfer of prescriptions; and a nationally accessible, “cradle to grave” summary patient record called “the spine” (figure). The provision of electronic functions at acute trust level form part of the NHS care record service, a collective term for all aspects of clinical IT support applications, from clinical decision making tools to digital x rays. The output of these applications is intended to be a health record that can be shared. The NHS care record service replaces the earlier twin concepts of lifelong electronic health records and local electronic patient records.1
Outline of national programme for information technology (NPfIT)
We are studying the processes and outcomes of implementing the NHS care record service in four acute hospital trusts in England. This involves assessing the local context in each trust, in depth interviews of staff and patients over a two year period, and a quantitative analysis of the effects of implementing three electronic functions of the record service. In this paper, we report findings from each trust's baseline assessment and information gathered from the first round of interviews.
Methods
We collected baseline information by meeting key IT, finance, and clinical directorate staff and reviewing documents and routinely published data. Interviews are taking place in three stages, with stage 1 interviews (the focus of this paper) taking place twice, at the start of the project and 18 months later. These interviews concern the development of NHS electronic patient records. (Stage 2 and 3 interviews investigate how electronic functions are experienced by staff and affect working practices and how they affect patient care.) The data reported here are from the first round of stage 1 interviews, with 23 senior managers and clinicians from the four trusts.
To enhance the generalisability of our findings, we selected the four trusts to reflect a range of characteristics (differences in size, number of sites, performance indicators, and financial situation) and various stages of implementing electronic health records. Participants included all local senior management staff involved in implementing the NPfIT, including the chief executive, director of information technology, medical director, and director of nursing.
Semi-structured interviews were conducted on a one to one basis at each trust by a qualitative researcher. We developed the interview framework by drawing on literature concerned with installing electronic patient records to identify key constructs.12–14 Topics discussed included the processes and outcomes of implementing electronic healthcare systems and the impact of the NPfIT policies. Interviews were recorded and transcribed.
Data analysis
We analysed the interview transcripts in three stages based on grounded theory principles of coding and theme abstraction15 rather than strict adherence to the theory of Glaser and Strauss.16 Literature on organisational change suggests the context and processes of change will be multilayered and complex.17 We explored this complexity by examining variations within and between the four trusts, taking account of organisational changes relating to NHS policy. We then grouped emerging themes according to the context (each trust's characteristics) because “analysis of change needs to attend to the interplay between processes, people, and events both internal and external to the organisation.”18 We explored the relations between each trust site and the wider organisation, between the organisation and the individuals within, and between individuals and the technology. Two members of the project team (JH and NF) independently read the interview transcripts to agree on emerging themes.
Results
The table shows the baseline characteristics of each trust, including level of implementation of existing electronic patient records and the expected date for replacing the patient administration system, the first step in implementing the NHS care record service. Data from the first round of interviews show the potential impact of these factors on implementing the care record service.
Table 1 Characteristics of the participating trusts
Multiple sites within trusts
Two of the trusts have multiple sites, resulting from recent mergers, and problems of poor communication and coordination between sites remain. Differences in working practices and organisational culture seem to have created tensions that may make the job of getting ready for the NHS care record service especially challenging (see box 1). Major changes resulting from the recent mergers seem to have affected staff morale, increasing the likelihood that staff will become resistant to the changes required during implementation.
Box 1: Issues of multiple trust sites and change overload
“There's the difference in cultures between the two ends of the same trust, the culture where the whole senior management team transported themselves over. And so I think at one end within the trust, the [name] end, the clinicians and the nurses and others are all used to a different way of working, which the people here are not. So I think there is a big difference actually between—if you ask people at that end I think you'll find a very different philosophy there.”—Clinical director, trust 2
“One of the things that definitely makes life much easier is that we're a single site organisation, so there is a single culture around this place; we're not a difficult political being with eight or nine hospital sites spread around. From an IT point of view that's very difficult to support and manage.”—IT manager, trust 4
“So, like I said, I think the organisation, leaving aside the IT, has quite a few issues still in terms of the changes it's gone through. Then add in the national programme and that's just, just another thing on top, and that's going to affect working practices across the whole organisation… It is yet another change, and I think certainly people are fed up of change and people do identify the national programme as being yet another IT project that is probably not going to work, that's going to cost a great deal of money, and why should they really cooperate with it?”—Clinician involved in development of electronic patient records, trust 1
Box 2: Issues of communication with NPfIT headquarters and lack of clinical engagement
“So I think we've not had, you know, we had some of the interaction, and I think what we've been asking for is clarity about, um, getting things done, what isn't coming, things like. There was really something last week about… the radiology systems, about the radiology information system and PACs, and in the application there's no radiology information system, there's just PACs.”—Executive director, trust 2
“The communication has been appalling, absolutely appalling. They've done some wonderful events, and I've met some people who are great, NPfIT, who are very facilitative and very enabling, and the next week you're told you're not allowed to talk to them. I've been to some meetings where I've met people who are very very good, and we've been ordered not, instructed, they've been ordered and we've been instructed that it's inappropriate to talk to them.”—IT manager, trust 4
“Despite what people say there's a lack of, there's a lack of engagement and, you know, even as chief executives, I think we've been involved and been asked to promote something they, we're promoting—we say it's a bit like trying to go and sell, probably in IT terms, vapourware and that's really what it felt like.”—Chief executive, trust 3
“I would say that the clinicians are sort of waiting to see what's going to happen before they commit themselves.”—Assistant director of nursing, trust 4
Communication between the national programme for information technology and the NHS
The lack of clarity from the NPfIT about future developments—with poor communication between NPfIT headquarters, the local service provider, and trust managers—was reported to be a major concern in all four trusts. Managers felt that local needs and advice have been ignored and expressed sentiments in interviews of feeling ignored, being “done unto,” and disempowered (box 2). Participants' views suggest a divide between the central NPfIT office and trusts, with the latter perceiving the former as failing to understand local issues. This lack of communication seems to have filtered down, with managers reporting a reluctance to communicate the benefits of the NPfIT to front line staff without having answers to questions about what IT services will be supplied and when (box 2).
Financial circumstances of trusts
Two of the trusts have substantial financial deficits, which were reported as contributing to slow progress on local IT projects (box 3). Central funding does not cover all of the costs of implementing the care record service, and local IT spending must be sustained or increased to provide the infrastructure necessary to support it.19 For participants, funding for the change management associated with the care record service was a key concern. Up to March 2004, instead of increasing spending, participants in “cash strapped” trusts reported that scheduled IT implementation had been halted to await details of the NPfIT to be made public (box 3). Understandably, trusts may be reluctant to spend on IT if some of the cost will be covered centrally. This lack of certainty seems to have created “planning blight,” with participants reporting that few IT initiatives have been championed (box 3), thus potentially widening the IT gap between “cash rich” and “cash poor” trusts.
Performance ratings
For trusts with a low performance rating (0 or 1 star), improving this rating was reported as a pressing concern (box 4). (Although the future of performance ratings is under review, performance indicators are likely to continue to be a key focus for trust managers.) Benefits of the NPfIT (which has a 10 year roll out), such as financial savings and improved patient care, will not be realised until after money has been spent on implementation. This will probably require investment in staff training as well as the IT infrastructure, perhaps temporarily reducing staff time available for clinical care. Trusts are likely to avoid any activity that decreases rather than increases productivity unless sufficient extra financial and human resources are provided (box 4).
Box 3: Issues of financial deficits
“I mean our first, our number one priority in this trust been stated by the [chief executive], and is quite clear to anybody, is money. We have to claw back our deficit, a huge deficit; [name] has an ever bigger one, and we are a very, um, broke strategic health authority, actually, but particularly this local health community. We're very strapped for cash, and we have to find millions and millions of pounds worth of saving this year alone and indeed over the next three years.”—IT and NPfIT project manager, trust 3
“And we have a senior management that have too much on their plate to cope with at the moment, and EPR [electronic patient records] and IT, as well as between [large figure] million pound underlying deficit. We're certainly not a trust that can invest from our own resources.”—Medical director, trust 1
“We've made real progress, um, in the development of our EPR programme, and those who've done so much work in that particular programme are naturally quite distressed if our particular EPR programme is simply going to go on hold for two, three, or four years, while we wait for a national programme to be implemented.”—Medical director, trust 1
“You know, the abandonment, the abandonment of the EPR has had an affect on people's desire to get involved too much in that way—let's wait until a bit later… I think there's a ‘Let's just not invest too much time’ attitude at the moment and see how it goes from here.”—Assistant director of nursing, trust 4
Supporting “legacy” IT systems
The NHS has traditionally devolved IT procurement, resulting in a proliferation of IT architecture. This approach contrasts with centralised standard setting and procurement under the NPfIT. Potential legacy problems reported by participants are the loss of existing electronic functionality and concerns over support for existing systems during any transition period.
All trusts in our study reported having highly effective customised pockets of IT. If these systems cannot be integrated with national “standards” some functionality may be lost (box 5). Loss of existing IT function may stall progress and is likely to beresisted. IT literate clinicians in our sample reported working hard to develop systems that best support their needs and the needs of their patients (box 5).
Box 4: Issues of performance ratings
“At the moment, you know, a lot of chief [executives], a lot of your short term focus is on star ratings and performance management because that's where, you know, the carrot, that's why you're driven down that route. So, you know, we're paid to do that and keep the strategic vision going, but it depends how much pressure you get about where your focus could be.”—Chief executive, trust 2
“So if that national programme wants this to happen they, the government, whoever, must make sure any moneys that come down through whatever route are ring fenced, and they're ring fenced right down to trust level, so that creative finance directors and others cannot divert them for other purposes.”—IT and NPfIT project manager, trust 3
Replacing existing systems will require contracts with existing suppliers to be redrawn. Maintaining goodwill and continued support for such systems may be difficult. Trusts that actively pursued the original plan for electronic patient records1 may be particularly disadvantaged if they are bound into long term contracts with suppliers not awarded contracts under the national procurement process.
Timetable for replacement of patient administration systems
To implement the care records service software, most trusts will need to replace their existing patient administration systems. The new administration system will act as a foundation on which additional “bundles” of clinical functions can be added. However, patient administration systems cannot be replaced immediately in all trusts. For example, in London this activity alone is projected to take up to five years. The timing of this replacement is causing concern, and participants reported that their trusts have been jostling for a slot that meets their particular needs (box 6).
Some trusts have reported an urgent need to replace existing IT systems for radiology or pathology. According to participants, the previously scheduled implementation of such replacement systems has been put on hold until details of the NPfIT have been made public (box 6). Such delay may mean a risk of system failure, but buying a temporary solution is seen as costly. Being first in the queue for implementing the care records service may increase the risk of delays and teething problems, with details of forthcoming support from the local service provider for change management still unclear. However, being at the end of the queue may lead to “planning blight,” with no new local IT development until the new administration system is provided (box 6).20
Box 5: Issues of loss of functionality and resistance from clinicians
“There's a feeling of loss of autonomy, um, and possibly lack of or loss of functionality, because some of the systems that we've got are, have been developed over a period of time, and they're pretty well customised and people get used to that level of customisation.”—Chief executive, trust 4
“Where it needs tailoring to local trusts—I don't think that's being listened to at all, and that's where they're going to find the biggest amount of resistance, which is where local systems will always be better than the national solution.”—Electronic patient records and NPfIT programme manager, trust 2
“Our ITU consultant writes programs: he wrote the ITU one here, and he's writing us a little program for duty doctor handover. It's like swimming in treacle to get it integrated into our system. You can't get it if you're in a, you know, in a regimented system that is becoming increasingly.”—Medical director, trust 1
“If we're saying to people, ‘You have to drop what you've got to a lower function,’ well that's going to be very hard to sell.”—IT director, trust 4
“Until we can get that level of functionality built into the national solution nobody is going to use it, well not from our trust anyway.”—Electronic patient records and NPfIT programme manager, trust 2
“So, yeah, they may have been working overtime developing their own system and now are being told, ‘No, you can't use it.’ And you have something which isn't as good or doesn't allow as much functionality or flexibility perhaps as something else.”—Research and development business manager, trust 2
“As a taxpayer, I'm furious, as a clinician who's dedicated time speaking on behalf of other professionals who've spent hours of unpaid time trying to make this work, they feel devalued, marginalised, and ignored. So there's enormous anger in this organisation, particularly at [name], with the way in which we've been dismissively treated.”—Medical director, trust 1
Discussion
The national programme for information technology promises far reaching benefits for patients and throughout the NHS.21 The immediate hurdle is the disruption and change that NHS staff must undergo during implementation of the NPfIT. Persuading people that “it will all be worthwhile” is at least as great a challenge as the technical one.
Doubters need to reflect on alternatives. Not investing in IT is not an option.19 22 The choice lies between a centralised approach like the national programme or more piecemeal local solutions. The benefits of the former are potentially much greater, but realising these benefits depends on procuring systems that work and managing their implementation without alienating staff. It is in these areas that our study has identified room for improvement.
Our study suggests that NPfIT project managers need to address four key issues:
Box 6: Jostling for a new patient administration system (PAS), concern over delays, and “planning blight”
“And so, obviously everybody wants the [new] PAS straight away, and you're obviously in the queue for that with everybody else.”—Divisional manager, trust 4
“It's going to be an absolute scrabble, you know, and I'm a bit annoyed. We went to a launch day for the, for the [local service provider] and one of questions I said, ‘You know, there's 77 trusts, a limited number of slots [for PAS replacement], you know, it is going to be a big bun fight.’”—IT director, trust 4
“If we aren't one of the first PASs, which I don't think we are, it could be 2010 or something before we even get a PAS, and then, you know, we've got to implement all the various compliant systems. So it could be a, over a decade before anybody, you know, and it will be over a decade in some places before anybody at some trusts see any difference.”—Chief executive, trust 4
“Our biggest sort of stumbling block for taking anything from NPfIT is the fact that nine times out of 10 we've got to have the [new] PAS in, so, as much as we would like to take some of the modules, we can't”—Electronic patient records and NPfIT programme manager, trust 2
“It's, well, it's been delayed basically. I mean in implementation, purchase and implementation of the system by a year and a half, I think, while we're inevitably waiting for the [local service provider] to be sorted, and now we're waiting for the process to go though… It's a bit of a mish-mash going on there, I must say. Um, I think, you know, you've got to kind of look at your local priorities in this case and say, ‘We need a new system in for risk factors and for managing demand and recording data better, um, and we need to go ahead and purchase as soon as we can.’”—Divisional manager, trust 4
“NPfIT for London said, ‘No, you have to do it this way.’ And it's not, it's just not up for negotiation, it is a very centrally driven mandate. ‘You will take PAS, you will take some minimum orders that include maternity and theatres, and then you can take some prescribing and some pathways.’ So, we were definitely aiming to do the clinical end of things first… it is frustrating because that's—you're right, in terms of strategy we did not want to do our PAS next and we did not want to do theatres and maternity.”—IT director, trust 4
Trusts vary in their circumstances, which affect their ability to implement the NPfIT
The process of implementing the NPfIT has been suboptimal, leading to reports of low morale among NHS staff responsible for implementation
The overall timetable for implementation is unrealistic, and trusts continue to face uncertainties. The need to renew the patient administration system in most trusts represents a bottle-neck, with timings published in the NHS Care Record Service: Indicative Deployment Plan23 not tying in with promises of detailed electronic patient records being provided by the end of 200724
Short term benefits alone are unlikely to be sufficient to persuade NHS staff to support the NPfIT wholeheartedly, particularly if local IT functionality is reduced.
Limitations of study
These issues were communicated to us by interviewees, with supporting information that showed their importance to the participating trusts. In these circumstances the validity of our findings is not in question, but the small number of cases makes us cautious about generalising more widely. In support of the generalisability of the study, however, the circumstances of participating trusts that were often the basis of managers' concerns are prevalent throughout the NHS: such as poor performance ratings (26% of acute trusts have < 2 stars),25 having a financial deficit (18%),26 or having recently merged.27 These issues did not necessarily coincide in the participating trusts, supporting the view that they are independent. Where the same issues occur in other trusts, we would expect them to have a similar impact. The main limitation of our study is that we may have missed important factors because they were not present in our participating trusts. Therefore, we cannot conclude that the issues highlighted in this report are the only or most important ones.
Implications for the national programme for information technology
NPfIT project managers can argue that these are still early days for the national programme. However, the views of senior NHS staff in our study represent a warning of the challenges ahead. The process of implementation needs to change rapidly for NHS staff to feel optimistic and to embrace IT changes with enthusiasm. Moreover, attributing benefits unequivocally to the NPfIT is likely to be difficult and to take time.28 29
Experiences of IT implementation in the UK12 and other countries confirm the importance of sociocultural considerations. A case study from Australia described a major failure of IT implementation, identifying organisational and cultural factors that led to the failure as well as technical ones, with the system failing to meet staff expectations.9 In the United States introduction of the “computer physician order entry” led users to feel that their work was disrupted and not facilitated and that the organisation gained more than they did,30 with reports of an adverse impact on team relationships.31
There are also major technical and logistical challenges to implementation, but NPfIT project managers have shown commitment to dealing with these.32 However, the sociocultural challenges are equally daunting,33–35 and we found that senior NHS staff felt these to have been neglected. One concern is that staff will not experience tangible benefits in the near future,6 36 but will have to cope with disruption, uncertainty, and change, and possibly a loss of IT functionality in the short term. In these circumstances, a more sophisticated approach is needed to gain the cooperation of front line staff, on whom success will depend.
What is already known on this topic
The NHS has invested heavily in a 10 year national programme for information technology (NPfIT)
What this study adds
It is too early to assess the success of the programme, but interviews with trust staff responsible for its implementation have identified concerns
Unrealistic and shifting timetables, lack of consultation and communication with NPfIT managers, and lack of perceived short term benefits have affected staff morale
Optimal delivery of the NPfIT will depend not only on technical capability but also on managing implementation so that staff embrace the IT changes with enthusiasm, and NPfIT headquarters urgently needs to focus on the latter
What might be the features of such a revised approach? It is clear from our interviewees that better communication is essential. However, improved communication could imply one way traffic (from NPfIT headquarters to trusts), and this alone is unlikely to win cooperation. An improved sense of realism would be a start, such as reconciling the overall timetable with the recently published schedule for replacement of patient administration systems across trusts.23 Representative users of the NHS care record service in trusts must become partners in the enterprise through genuine consultation; this is what is likely to give them a sense of ownership and reward as systems are introduced, even when the going gets difficult.
Conclusion
We recommend that NPfIT headquarters urgently revisit its priorities, managing the changes in working practices in addition to the technical challenges. The NPfIT is likely to succeed or fail according to the groundswell of opinion, as well as its technical performance (unless the latter is catastrophic). Over the next five years, the NPfIT implementation will be seen either as a glass half full or a glass half empty. In the words of one chief executive, “This isn't the end of things by any means. In 10 years time, when they say, ‘IT system disaster.’ That's what will happen, won't it? You can see the headlines now. But underneath, it will say how things have improved.” Senior managers responsible for the NPfIT need to ensure that NHS staff see the glass as half full.
Acknowledgments
 Details of the interview framework appear on bmj.com
Details of the interview framework appear on bmj.com
We thank the participating trusts for agreeing to be cases and individual interviewees for their time and interest in the study. We also thank members of the steering group for their continuing support and comments from the two BMJ referees.
Footnotes
-
Contributors JH planned, conducted, and reported the work. BCR, NF, and AH planned and reported the work. CM conducted and reported the work. NF is guarantor for the study.
-
Funding This project is funded by the NHS Service Delivery and Organisation R&D Programme (reference SDO/44/2003).
-
Competing interests None declared.
-
Ethical approval NHS Trent Multi-centre Research Ethics Committee and NHS Trust Local Research Ethics Committees.